Years ago Neil Stinson trained to care for Ebola patients. Now he is on the front lines of COVID.
“A bunch of us came from different ICU environments. We became a tight team, a great team, that came together very quickly.”
May 5, 2020
Neil Stinson has been a pediatric emergency room nurse for a number of years. Last year he became an intensive care nurse and joined the LifeFlight team at Vanderbilt University Medical Center. Lately, since he’s been working in Vanderbilt’s dedicated COVID-19 unit, he’s noticed that lots of people are paying attention to his job.
“I’ve had people I haven’t heard from in years call me and thank me for what I’m doing,” he says. He sounds as though he’s not quite sure what to make of that.
When word came that a pandemic was sweeping the world and that VUMC planned to set up a unit to care for its victims, Stinson, RN, EMT, was tapped to work in that unit, and it has been his work home for two months now.
It wasn’t the first time that Stinson had stepped up to care for people with a dangerous infectious disease.
“We’re here to take care of people who are sick and suffering. My professional style is to get out in front of situations. I wanted to be part of the reality rather than the fear.”
In 2014, an Ebola outbreak in West Africa resulted in several infected people coming to the United States and, in response, Vanderbilt formed its Communicable Disease Response Unit (CDRU), a group of volunteers who agreed to train to care for patients with potentially deadly infectious diseases. That included learning and practicing how to put on, take off, and work wearing the most advanced personal protective equipment (PPE).
“Plans got ramped up very quickly,” he recalls of that time. “We needed a team of experts and people who were willing — dedicated volunteers.”

Some members of VUMC’s Communicable Disease Response Unit show off their custom shirts.
That calling fit in perfectly with his vision of his role.
“We’re here to take care of people who are sick and suffering,” he says. ”My professional style is to get out in front of situations. I wanted to be part of the reality rather than the fear.”
Stinson’s reality these days is VUMC’s patient care unit on the eighth floor of Medical Center East, a newly remodeled area that was completed early this year.
A small number of COVID-19 patients were initially admitted to the Medical Intensive Care Unit at Vanderbilt University Adult Hospital, and a few continued to receive care there. But when it was apparent that a dedicated unit was going to be necessary to deal with the pandemic, a team of experienced ICU nurses, nurse practitioners, intensive care physicians and others came together quickly to staff that unit and make it a reality.
“A bunch of us came from different ICU environments,” Stinson said. “We became a tight team, a great team, that came together very quickly.”
Stinson knows that there is intense curiosity among the public about what life is like inside a COVID-19 inpatient unit.
Depending on the shift and the patient census, there are usually between five and seven nurses working per shift, in addition to the intensive care physicians, nurse practitioners, respiratory therapists, environmental service workers, dietary employees and others who also serve on the unit.
At Vanderbilt’s COVID-19 unit, there is an acute or ICU area down one hallway which, throughout the past few weeks, has usually had five or six patients. These are the most critically ill patients, and, depending on how stable they are, may require a patient-nurse staffing level of 1-2 or even 1-1.
There are other patients on the unit who are obviously quite sick and need to be hospitalized, but who are not depending on a ventilator to breathe and are conscious and able to talk.
What Stinson describes as normal workplace routine happens to be in a high-stress workplace where everyone there, no matter what job they’re doing, is striving to help very sick people get better while staying safe themselves.
The 12-hour shift begins with a huddle for any new staff, then the handoff and report, where incoming staff learn what’s been going on over the past shift and what is anticipated for the next few hours. The physicians and nurse practitioners round on their patients.
“The routine is standard for an ICU,” is the way Stinson describes it.
Except for the PPE, of course, which is on everyone’s mind all shift long.
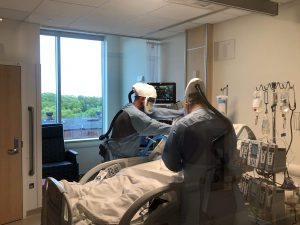
While some staff work in protective gear in patient rooms, others are available to assist with needed supplies.
At the beginning, each person does a PPE check — do they have everything they need for protection against infection? For those working on the intensive care side, where many of the patients are intubated, enhanced precautions must be observed, PPE includes gown, gloves, mask, and face shield, and sometimes a PAPR, which includes a pressurized hood with a full face shield.
It’s a lot to put on and a lot to take off, and doing that a minimum number of times per shift is more efficient in use of both time and supplies.
And then, there’s the coordination required so that not everybody is in full PPE at the same time. Some staff members need to be available for other tasks on the unit, including retrieving supplies for caregivers who are in PPE. Thought has to be given to what each patient needs, and on what schedule.
And, of course, what Stinson describes as normal workplace routine happens to be in a high-stress workplace where everyone there, no matter what job they’re doing, is striving to help very sick people get better while staying safe themselves.
Stinson says a transition period between his work and his family is essential.
He speaks with admiration in his voice for his coworkers: Kim Carter, RN, manager of the COVID unit who also was part of VUMC’s Communicable Disease Response Unit; Susan Bosworth, CDRU educator and coordinator; and Kristin Nguyen, RN, and Cody Hamilton, RN, both of whom came to the COVID unit from MICU.
He also mentioned Jerusha Robinson, RN, and Maddie Hayes, RN, who have been with some COVID patients in the last moments of their lives. “They have endured a remarkable emotional load,” he says.
The Medical Intensive Care Nurse Practitioner team, called Team Green, have stepped up to be the medical providers, meeting the needs of patients who are the sickest of COVID-19. Stinson notes that the team has not missed a beat and have risen to the occasion.
How does Stinson deal with the emotional load of his work, especially now?
He and his wife Lauren, a hospice nurse, have three children, aged 10, 6 and 4, and Stinson says a transition period between his work and his family is essential.
“The walk across campus after a shift is quite soothing,” he says. “I come down and decompress. I listen to music or a podcast on the way home, but it’s also good to take a few moments to think about what you’ve been doing.”
Especially since he and his wife both work in health care and are around others as part of their jobs, they both now make it a practice to enter through the basement of the house and shed their work clothes before coming upstairs. Their kids are accustomed to when dad and mom first get home from work, they’re in their underwear.
“The kids have learned not to run and hug us first thing,” he says.
He thoroughly washes his hands, puts on clean clothes, and then, as he puts it, “I try to concentrate on being home.”
As some of the “stay at home” orders are loosened, Stinson joins the rest of us in watching the next few weeks with interest and a little trepidation.
“Nobody knows what’s going to happen,” he says. “It’s so dependent on human behavior.”
But he does have some advice, both as a person who goes to work in a COVID-19 unit and as the parent of three children: “If you think, ‘Should I wash my hands now?’” he says, “The answer is yes.”

Teamwork in the face of a difficult and changing circumstance, all to benefit the patient, is a hallmark of the COVID unit. All photos courtesy Neil Stinson.










